Table of Contents
Mohs Surgery: The Gold Standard in Skin Cancer Treatment

Getting a skin cancer diagnosis is scary. As soon as you hear the word “cancer,” it’s common to think about the worst-case scenarios.
Fortunately, most skin cancers are completely curable. If detected early and treated appropriately, we’re able to significantly reduce the recurrence rate of many types of skin cancers and send patients home skin cancer-free.
That said, the prospect of Mohs surgery to remove skin cancer, especially on cosmetically and functionally important areas of the face and body, can be an intimidating thought for many individuals.
“Many patients come to me with concerns about scars, recurrence, the size of the defect, and whether they will repeatedly need Mohs now that they have had one procedure,” shared Dr. Mark Abdelmalek, Board-Certified and Fellowship-Trained Mohs Surgeon.
Getting answers to your questions and understanding your options can help to alleviate the anxiety that comes with this unwelcome diagnosis.
“I am happy to be able to reassure patients that the majority of skin cancers we treat with Mohs surgery are not life threatening skin cancers. It is important, however, to treat skin cancers because they can become locally aggressive,” Dr. Mark continued, “If left untreated the skin cancer will eventually become a spot that bleeds on a regular basis.”
Mohs surgery is the recommended course of treatment for the vast majority of skin cancer diagnoses.
“Mohs offers the highest cure rate and best outcomes for skin cancer,” Dr. Mark shares, “It allows us to remove all of the skin cancer, but leave as much of the normal cells behind, allowing for the smallest scar and best cosmetic outcome.”
In this guide, we cover what Mohs surgery is, which types of skin cancers can be treated with Mohs surgery, how to select the best Mohs surgeon for ideal surgical outcomes, and what to expect before, during and after your procedure.
What is Mohs Surgery?
Mohs surgery is a highly-specialized surgical treatment named after its founder, Dr. Frederick Mohs. The American College of Mohs Surgery was founded in 1967, and for decades, has been the most advanced, precise, and effective treatment for the removal of skin cancer.
Mohs involves surgically removing skin cancer layer by layer and examining the tissue under a microscope to ensure the tumor is removed entirely and only healthy, cancer-free tissue remains. It is a patient-centered approach and unique procedure in that it allows surgeons to remove all of the skin cancer while leaving as much normal tissue in the skin as possible.
It has proven to be the gold standard for treating many types of skin cancer, including basal cell carcinomas (BCCs) and squamous cell carcinomas (SCCs), the two most common types of skin cancer.
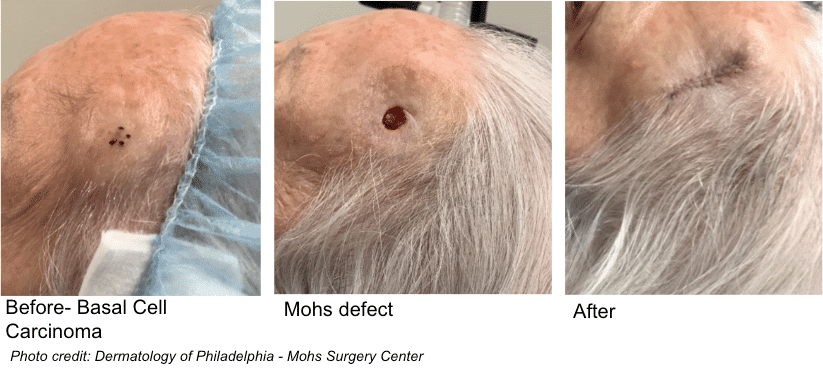
Basal Cell Carcinoma (BCC)
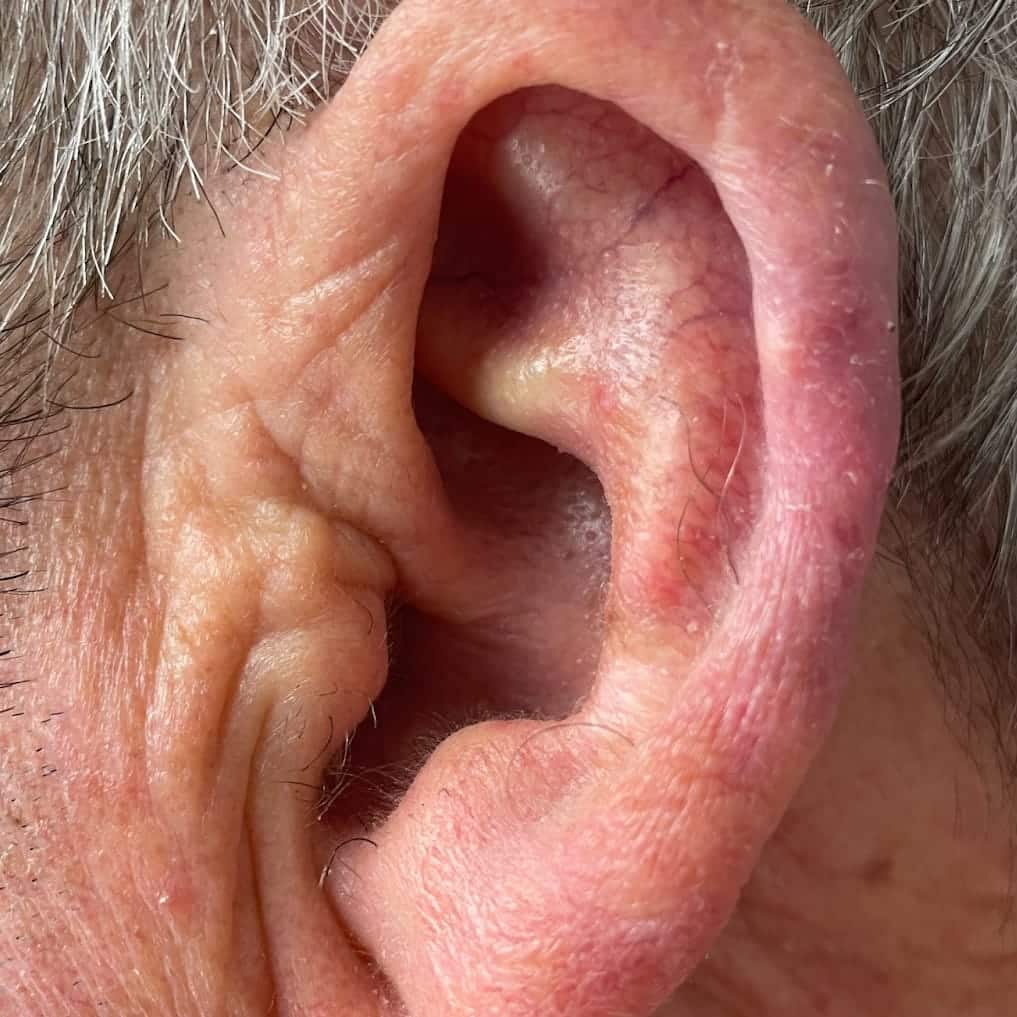
This is treatable skin cancer, with more than 3 million US cases per year. This type of skin cancer begins in the basal cell layer of the epidermis, the top layer of skin, and often appears as a pink or red spot, a bleeding sore that does not heal, a pearly pink bump or a waxy white spot on sun-exposed areas. They are most often on the face and neck, but can appear anywhere on the body.
Squamous Cell Carcinomas (SCC)
This is the second most common skin cancer, with an estimated 1.8 million US cases per year. This type of skin cancer begins in the higher levels of the epidermis, the outermost layer of skin, and usually appears as a scaling pink or red sore, a crusted spot that does not heal, or a thickened rough, raised area. If detected and treated early, this is treatable skin cancer.
If you’ve been diagnosed with melanoma (lentigo maligna), a staged excision, also known as slow Mohs, is often the recommended treatment. Contact our office today to discuss your options for the treatment of melanoma.
Mohs Surgery: The Highest Cure Rate
The roots of skin cancer may extend beyond the visible portion of the tumor. If these roots are not removed, cancer will recur. “Often what is visible above the skin is kind of like the tip of the iceberg,” Dr Mark advises.
The Mohs surgery process was developed to reduce and nearly eliminate the chance of recurrence, offering the best surgical outcomes and the highest cure rates for skin cancer compared to other treatment methods.
Mohs Surgery offers a cure rate of up to 99% for most tumors. The roots of skin cancer may extend beyond the visible portion of the tumor. If these roots are not removed, cancer will recur. “Often what is visible above the skin is kind of like the tip of the iceberg,” Dr Mark advises.
The precision of Mohs surgery allows the examination of 100% of all surgical margins to ensure that all of the skin cancer is examined and removed. The Mohs and specialized reconstruction techniques also maximize the aesthetic result after skin cancer removal with the smallest scar possible.

Is Mohs Surgery Right for Me?
If you’ve been diagnosed with the most common forms of skin cancer, you may be asking: Is Mohs surgery right for me? The answer is, in most cases, yes. When detected and treated early, nearly all skin cancers are completely curable with Mohs surgery.
Mohs surgery may be the best option for you if you’ve been diagnosed with basal cell carcinoma (BCC) or squamous cell carcinoma (SCC), especially if your cancer is located in cosmetically and functionally important areas of the face (eyes, lips, nose, ears and scalp) or on the fingers, toes or genitals.
Mohs surgery is also recommended if your skin cancer tumors are large, aggressive or growing quickly, if they have indistinct edges or have recurred following previous treatments.
Patients are referred for Mohs micrographic surgery because it is considered the most effective treatment option for these locations and types of cancers.
Why Choose a Fellowship-Trained and Board-Certified Mohs Surgeon?
While Mohs micrographic surgery is the gold standard of skin cancer treatment, the surgeon you select for your procedure can influence the outcome. It is your right to understand the differences between available surgeons, certifications and expertise.
Dual Boarded Dermatology and Mohs Certification
Not all surgeons who perform Mohs Surgery are board-certified in Mohs Surgery. An American Board of Dermatology (ABD) board-certified dermatologist has undergone extensive training and has advanced knowledge of medical, surgical, and cosmetic treatments. Some Mohs surgeons, like Dr. Mark Abdelmalek, are dual-board certified in Mohs Surgery and Dermatology.
Mohs Board Certifications
Recently the American Board of Dermatology was approved by the American Board of Medical Specialties (ABMS) for a new board certification in Micrographic Dermatologic Surgery (MDS). To become board-certified in Mohs surgery (MDS Certification), candidates must hold primary certification in general dermatology from ABD and demonstrate experience in the subspecialty. Dr. Mark Abdelmalek was in the select first group of Mohs surgeons in the country to earn board-certified status for Mohs surgery.
Fellowship-Training in Mohs Surgery
To become a fellow with the prestigious American College of Mohs Surgery (ACMS), dermatologists must complete an intensive surgery fellowship training under direct and close supervision by an experienced Mohs surgeon. The ACMS or “Mohs College” was founded in 1967 by Dr. Frederick Mohs himself. Members who complete 300 Mohs surgery cases and go through an application process can achieve “fellow” status in the American College of Mohs Surgery.
An ACMS Fellowship-trained Mohs surgeon has extensive experience performing complex wound reconstruction and removing tumors in difficult locations. By choosing a fellowship-trained and board-certified Mohs surgeon, you can rest assured that you will receive the highest standard of care from an experienced surgeon.
Years of Experience
Selecting a surgeon with extensive years of experience managing complex Mohs surgery cases helps to further ensure ideal outcomes. Dr. Mark has performed tens of thousands of dermatologic and Mohs surgeries and is highly regarded by his peers for excellent surgical and reconstructive techniques.
Click here to see if your Mohs surgeon is fellowship trained.
Dr. Mark Abdelmalek: Intensive Training & Extensive Experience
Since 2007, Dr. Mark Abdelmalek has specialized in Mohs surgery, acquiring extensive experience and treating thousands of skin cancer patients with complex Mohs surgery cases.
Dr. Mark is dual board-certified in Mohs Micrographic Dermatologic Surgery and Dermatology. He is a Fellow of the prestigious American College of Mohs Surgery. He is a fellowship-trained dermatologic surgeon who has completed additional surgical training beyond traditional dermatology training. As such, he is specially trained in surgery, pathology, and reconstructive surgery.
How to Prepare for Mohs Surgery
Start with a good night’s sleep before your Mohs surgery day, and eat a light breakfast on the day of surgery.
No makeup or jewelry should be worn if surgery is to be performed on your face. Bring a good book or magazine with you, as you will spend a significant amount of time waiting while the microscopic slides are prepared and interpreted. We offer the music of your choice during Mohs surgery, and studies have shown that playing music you like can lower your anxiety levels on the day of surgery. We have a coffee bar and snacks while you are waiting. You may want to bring a light lunch as you may spend most of the day with us on your Mohs surgery day. We have a refrigerator in our waiting area if you need it.
Medications & Mohs Surgery
Most medications, including blood thinners, can be continued before your surgery. However, please let us know what blood thinners you are on as taking them can increase the risk of. If you are currently taking medication, continue as usual unless directed otherwise by your physician. If you are prescribed blood thinners by your doctor please do not stop these without talking to your doctor.
If possible, please avoid medications containing ibuprofen, commonly found in Advil, Nuprin, Naproxen, and Motrin, for at least three days before surgery. If you need a pain reliever, we prefer you take acetaminophen, which is found in Tylenol.
If you have been told by your dermatologist to use medications such as Efudex, Carac or Aldara, we ask that you not use these topical medications anywhere on your body for two weeks before or two weeks after Mohs surgery. Using these medications can slightly increase the risk of a surgical site infection.
What to Expect with Mohs Surgery at Dermatology of Philadelphia / Mohs Surgery Center
Many individuals are anxious to undergo Mohs surgery. However, when the procedure is complete, patients often share with us that it was better than they anticipated.
Day of Mohs Surgery
Your Mohs surgery will be performed as an outpatient procedure in our office. Shortly after your arrival, you will be taken to one of our treatment rooms. The surgeon will numb the tumor area entirely with a very small needle under local anesthesia.
Your Mohs surgeon, Dr. Mark, will then remove the first layer of tissue with a narrow margin of healthy tissue surrounding cancer. This step typically takes about 20 minutes, depending on the size and location of cancer.

From there, you will be temporarily bandaged and able to return to the waiting room to chat with the person accompanying you, read a book or step out for fresh air while the tissue is processed in our in-office laboratory.
Mohs Surgery Center Laboratory

By the time you reach the waiting room, the removed tissue will be in our Mohs laboratory.
Dr. Mark first brings the tissue to the tissue intake station, divided into pieces. The surgical team carefully draws out a map of the surgical site so that any skin cancer that remains can be precisely located.
Once the map is drawn, the tissue is processed in a cryostat, a machine that allows tissue to be kept at extremely cold temperatures. The piece of tissue is embedded onto a block, frozen, and cut into very thin sections. The tissue slices are placed on microscope glass slides and processed through a staining machine that stains the tissue with special stains to highlight the various cell types.
Each tissue section on the microscope glass slide is carefully examined under a microscope by Dr. Mark looking for any evidence of remaining cancer.
It takes about one hour for the tissue to be cut, frozen, dyed and made into microscopic slides for Dr. Mark to review.
Additional Layers Are Sometimes Needed
If examination of the microscope slides reveals that your tissue still contains cancer cells, Dr. Mark will identify the exact area of cancer on the “map,” and the procedure will be repeated to remove another layer of skin. Further tissue is removed only from the areas where tumor cells were found, using the map created. The process is repeated until there is no evidence of cancer remaining.
The average number of Mohs surgery stages required to clear a tumor is one to three. However, sometimes you may need more than 3 stages before your skin cancer is completely removed.
When surgery is complete, a decision will be made as to how to manage your wound. Because skin cancers can grow deeply and develop roots extending beyond the area you see, the final size of the surgical wound will be determined by the extent of your tumor.
How Mohs Wounds are Managed
Once it has been determined that your skin cancer has been completely removed, Dr. Mark will discuss with you options to manage your wound. The decision will depend on the size, depth, and location of your wound.
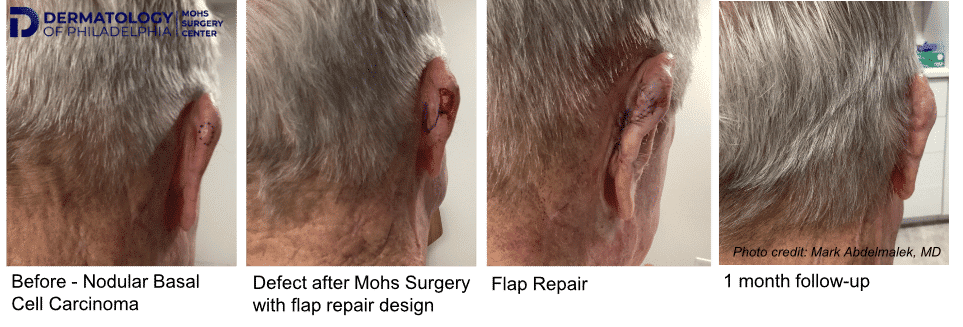
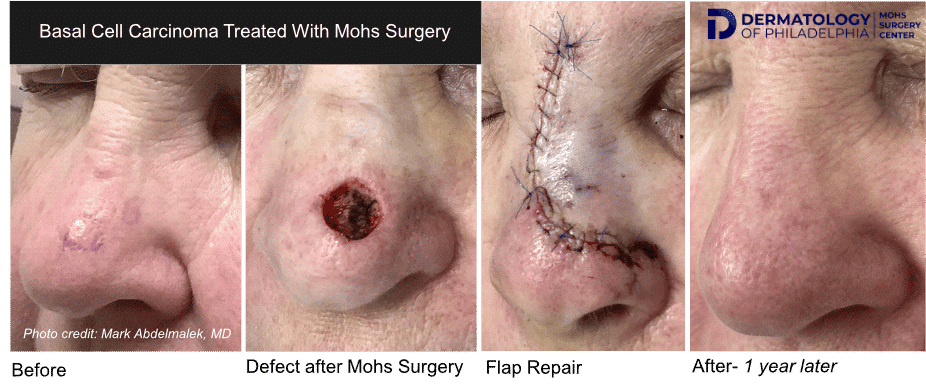
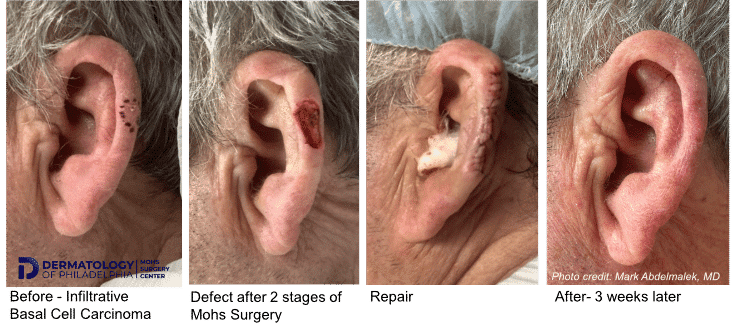
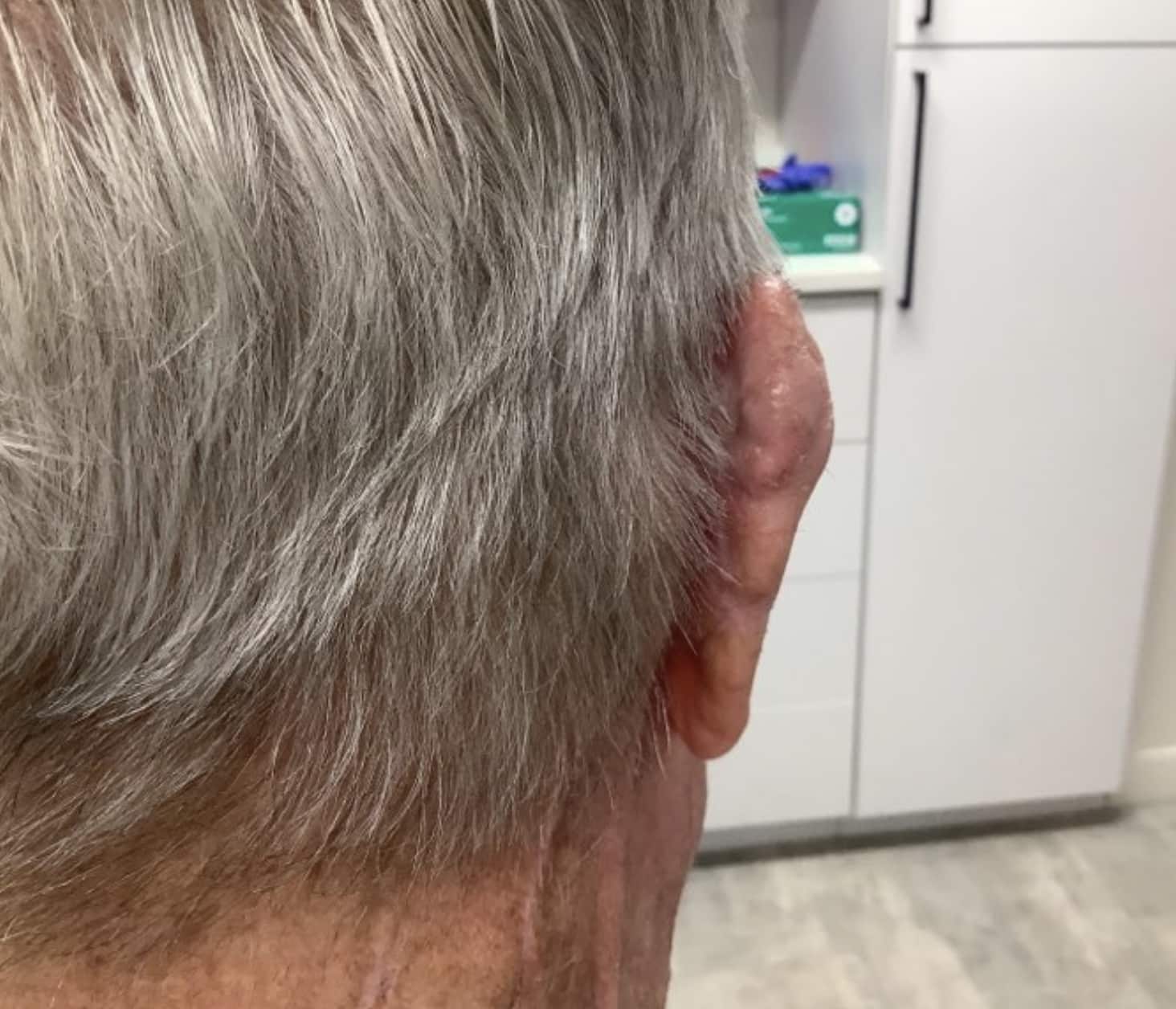
Healing by Granulation
In some instances, especially if the wound is shallow or on a concave surface, the wound may be allowed to heal by itself – this is called “healing by granulation” or by “second intention.”
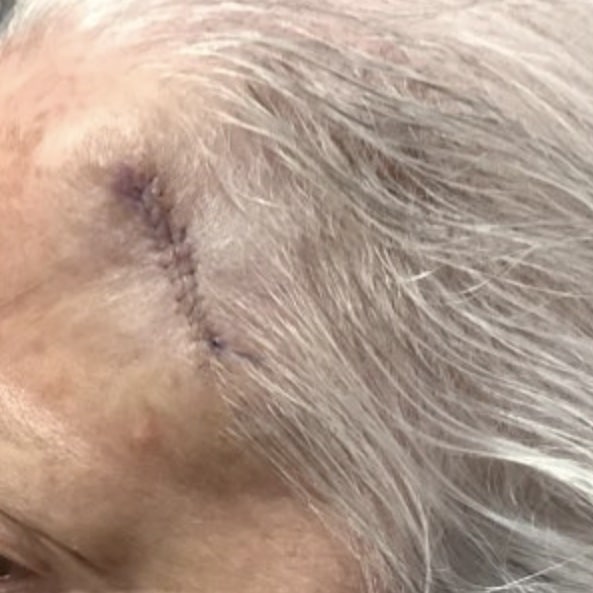
Same Day Repair by Dr. Mark
In most cases, the best option for closure is with stitches. In other cases, a skin graft or a skin flap from the surrounding areas is needed for reconstruction. If any repair is needed, the vast majority of the time this is performed by Dr. Mark the same day, immediately after obtaining clear margins.
Coordinated Repair
Rarely, depending on the size and location of the defect, Dr. Mark will work with trusted surgical colleagues from plastic surgery, oculoplastics, or head and neck surgery to coordinate a repair of the wound.
Reconstruction techniques continuously evolve and improve with innovative flaps and surgical repairs to maximize cosmetic outcomes.
Healing & Recovery After Mohs Surgery
If stitches are placed, you will likely be asked to return to the office for suture removal in 1-2 weeks. If your wound is left to heal by itself, you will need daily bandage changes until the wound heals, but we will likely want to see you for a wound check as well.
The time to heal varies by location. For example, it may be days to weeks on the face, but on the legs, it can take many weeks or even a few months, depending on the extent of surgery. In every case, you will be given written instructions on how to change your bandages for optimal healing post-surgery. Our office and on-call doctors are always available to you 24/7 after your surgery.
Understanding the healing process is helpful to relieve many concerns post-surgery. The following list outlines possible symptoms you may experience and how to manage them if they occur.
Pain
Most patients do not have severe pain but may experience slight discomfort. If this occurs, we suggest taking acetaminophen (Tylenol).
Bleeding
Occasionally, bleeding happens after surgery. If this happens, do not become alarmed. Lie down and place steady, firm pressure over the wound as close as possible to the bleeding area. Apply firm pressure continuously for 20 minutes (timed). Do not lift the bandage to check on the bleeding. If bleeding persists after 20 minutes of steady pressure, apply pressure for an additional 20 minutes. If bleeding continues, call our office at (215) 315-3197, or go to the nearest hospital emergency room.
Swelling
Swelling is very common following surgery, particularly when performed near the eye. All wounds swell a little. Usually, this is not a problem, and the swelling diminishes as the wound heals. Ice packs around a cloth may help to reduce the swelling. Sleeping with an extra pillow can also help with facial swelling. The swelling is often the worst 48 to 72 hours after surgery.
Drainage
All wounds drain to some extent during the first week or two. This is why dressing changes are necessary.
Infection
Infection of the wound is rare. However, if you see thick, foul-smelling fluid coming from the wound, please call our office immediately. Signs of infection to look for include increased redness, the warmth of the site, fever, and pain that is getting worse. An antibiotic may be necessary.
Redness
All wounds will develop some redness, which fades gradually. If the area becomes extremely red, it could be a sign of infection. If the area becomes red and itchy, you may be allergic to either the ointment or tape. Call our office if this condition develops.
Scarring
All surgeries will leave some scar. However, your scar will improve and become less noticeable as time passes. Fortunately, scars on the face heal better than any other place on the body.
What to Expect After Your Wound Appears Healed
Most patients have minimal to no issues after Mohs surgery. In some instances, you may experience some tightness as the wound heals. This is normal and usually lessens with time. Patients also may experience itching as their wounds are healing.
Frequently, the tumor and the surgery may involve nerves in your skin, and it may take up to a year, or even two years, before normal feeling returns to an area. In rare cases, the area treated can remain numb permanently, especially on the upper forehead and scalp.
The scar tissue around the wound contains more blood vessels than the surrounding skin in some people. This results in a red scar. This usually improves with time, and the redness gradually fades. Sometimes portions of the scar become thick, and this can be managed with local injections of a medication to reduce thickening. Lasers can also be used to decrease redness around a scar.
Very rarely, a scar is unacceptable. If this is the case, surgical scar revision may be considered. However, we usually advise patients to wait 6-12 months before performing a scar revision. This is because the scar continues to improve in appearance and becomes less conspicuous up to one year after surgery.
After Mohs Surgery
After Mohs, you will likely be asked to follow up for wound checks in 1 to 3 weeks. After that follow-up wound check, visits may be scheduled as needed.
Follow-up Visits with a Board-Certified Dermatologist
Once you have skin cancer, you have a higher risk of developing more skin cancers. We recommend you follow up with a board-certified dermatologist after your surgery is over, and your wound has healed. These visits can help with the early detection and treatment of new skin cancers that may develop as well as the rare recurrence of the skin cancer that was treated.
If you notice any suspicious areas on your skin between visits, it is best to check with your dermatologist to see if a biopsy is needed. If you are a patient of Dermatology of Philadelphia, contact our office to schedule an appointment to meet with a board-certified dermatologist.
References: 1. McGregor, Sean, DO, PharmD, 2015 Dec; Superficial Radiation Therapy for the Treatment of Nonmelanoma Skin Cancers
Alternatives to Mohs Surgery
The overwhelming majority of patients can tolerate Mohs surgery. However, a small subset of patients may benefit from alternative treatments.
Medical Management is an option Dermatology of Phialdelphia offers some patients for certain small and thin skin cancers that are not in high-risk locations. This could include various medications.
Photodynamic Therapy is an option Dermatology of Philadelphia offers some patients with superficial skin cancers, squamous cell carcinoma in-situs, that may be arising in pre-cancerous spots (actinic keratoses). Photodynamic Therapy may also be recommended if we feel the biopsy took care of the majority of a superficial skin cancer and there is not much left to see clinically.
Superficial Radiation Therapy (SRT) is an alternative option, often when Mohs surgery is not feasible. The American Academy of Dermatology and the National Comprehensive Cancer Network (NCCN®) consider superficial radiation therapy a “second-line option when surgery is contraindicated” or for “non-surgical candidates.”
When considering radiation therapy for skin cancer, it is important to know that radiation therapy is time-consuming, requiring multiple treatments over an extended period of time. Radiation also damages healthy tissue in the radiation path and increases the risk of developing additional skin cancers later. In contrast, Mohs surgery is complete in one day and has a very well-established safety profile.
An important distinction with Mohs surgery is proof that the cancer is cured with pathology. This is not possible with radiation therapy and there is never confirmation that the entire cancer has been removed once radiation is complete.
“Certain kinds of radiation treatments are sometimes added on as an additional treatment for certain high-risk skin cancers, but I do not believe superficial radiation therapy is ideal for the vast majority of skin cancers as a first line treatment,“ explains Dr. Mark.
The published recurrence rate for basal cell carcinoma with superficial radiation therapy is 4-16%. However, with Mohs surgery the recurrence rate is around 1-2%.
For squamous cell carcinoma, the published recurrence rate with superficial radiation therapy is 6 -11%. By comparison with Mohs surgery the recurrence rate is very low, around 2-3%.
“Those are big differences in cancer cure rates. Mohs surgery is the most effective treatment option with the highest cure rate for almost all skin cancers,” Dr. Mark said.
Schedule Your Mohs Surgery Appointment
TWO LOCATIONS TO CHOOSE FROM: VOORHEES, NJ AND CENTER CITY PHILADELPHIA
If you’ve been referred for Mohs surgery by your dermatologist, schedule a consultation or appointment with Dr. Mark at Dermatology of Philadelphia | Mohs Surgery Center today.
Fill Out the form Below or Contact our office at (215) 315-3197 to get started.
The Mohs Surgery Process





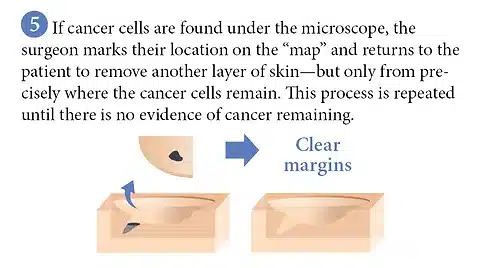

© American College of Mohs Surgery 2017 – All Rights Reserved